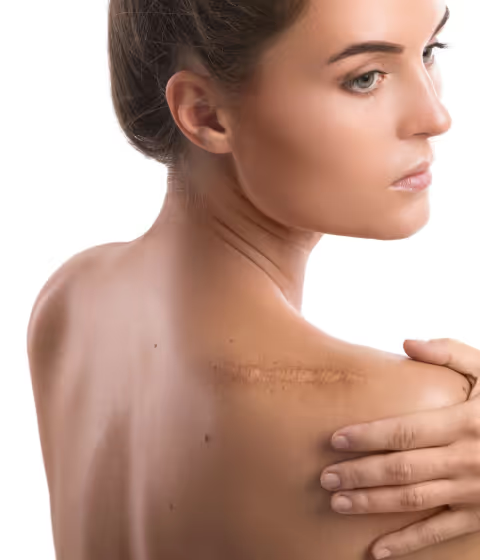
Are there certain areas of the body that are more difficult to treat for scarring?

Scarring outcomes vary significantly depending on anatomical location due to differences in skin tension and blood supply. At EmilMD, Dr. Kohan identifies high-tension areas like the chest and shoulders as the most difficult to treat. Specialized protocols allow EmilMD to manage complex scars effectively, ensuring patients achieve the smoothest possible skin texture across all body regions.
Table of contents
The human body possesses a remarkable ability to repair itself following injury, yet the quality of that repair is rarely uniform across different anatomical sites. When the dermis is breached by surgery, trauma, or inflammation, the resulting scar tissue is a functional patch rather than a perfect replacement of the original skin. Patients often notice that a scratch on the face heals almost invisibly, while a similar mark on the shoulder may broaden or thicken over time. This discrepancy is not a matter of chance but is rooted in the complex physiological and mechanical properties of various body regions.
Understanding why certain areas are more prone to problematic scarring is essential for anyone considering elective surgery or seeking revision of existing marks. Factors such as skin thickness, the density of sebaceous glands, and the proximity to underlying bone or muscle all play a role in the maturation of a scar. However, the most significant factor is often the amount of tension or movement the skin must endure during the healing process. Constant stretching pulls at the edges of a healing wound, signaling the body to produce more collagen, which can lead to raised or widened scars.
At EmilMD, the approach to scar management begins with a thorough assessment of these regional variables. Dr. Kohan recognizes that a scar on the back requires a different management strategy than one on the eyelid. By identifying high-risk areas early, clinical teams can implement preventative measures that guide the healing process toward a more aesthetic conclusion. This proactive mindset is what allows patients to undergo transformative procedures with the confidence that their final results will be as discreet as possible.
The Impact of High Tension and Motion on Scar Maturation
The most difficult areas to treat for scarring are those subject to high levels of tension and frequent range of motion. The chest, shoulders, and upper back are notorious for developing hypertrophic scars or keloids because the skin is constantly pulled during everyday movements like reaching, lifting, or even breathing. When the wound edges are under constant mechanical stress, the body attempts to reinforce the area by depositing excess collagen. This biological overcompensation results in scars that are thicker, redder, and more prominent than those found in quieter areas of the body.
Joints also present a significant challenge for scar revision and initial healing. Because the skin over the knees, elbows, and knuckles must stretch and compress thousands of times a day, maintaining the integrity of a fine surgical line is exceptionally difficult. In these locations, scars have a tendency to stretch out over time, becoming flat but wide, a phenomenon known as atrophic or stretched scarring. Managing these areas requires a combination of precise surgical closure and strict post-operative activity restrictions to minimize the mechanical forces acting on the tissue.
To help patients visualize how tension affects different body parts, the following list outlines the most challenging anatomical zones for scar management:
- The Presternal Region: The center of the chest is the most common site for keloid formation due to high skin tension and limited blood flow.
- The Deltoid and Shoulder: Constant arm movement makes this area prone to widening and thickening of surgical or traumatic scars.
- The Upper Back: Thick skin combined with the mechanical stress of torso rotation often leads to raised, firm scar tissue.
- Mobile Joints: Knees and elbows frequently experience scar stretching because the skin is under maximum tension whenever the joint is flexed.
- The Lower Legs: Poor circulation compared to the upper body can slow the healing process, leading to darker or more persistent scarring.
The biological environment of these regions further complicates the healing process. For instance, the chest has a lower density of certain blood vessels compared to the face, which can slow the delivery of essential healing factors. When blood supply is less than optimal, the inflammatory phase of wound healing may be prolonged. A longer inflammatory phase is a primary trigger for the excessive collagen production that characterizes difficult scars. At EmilMD, specialized dressings and tension-reducing techniques are employed to counteract these natural disadvantages.
Recovery in high-tension areas involves more than just waiting for the wound to close. It often requires months of consistent care, including the use of silicone sheeting or pressure garments to stabilize the tissue. Patients must be particularly diligent about following activity guidelines to ensure the scar has enough time to gain structural strength before being subjected to heavy loads. When these protocols are followed under the guidance of Dr. Kohan, even the most difficult areas can achieve a result that blends seamlessly with the surrounding skin.
The goal is to manage the body's natural response to injury. By understanding that the shoulders and chest are "high-risk" zones, the clinical team can tailor the surgical plan to place incisions along natural tension lines, known as Langer’s lines. This strategic placement ensures that the natural movement of the body actually helps keep the wound closed rather than pulling it apart. This level of anatomical expertise is a hallmark of the care provided at EmilMD.
Anatomical Variations in Skin Thickness and Glandular Density
Another factor that makes certain areas harder to treat is the inherent thickness and composition of the skin. The skin on the back and the soles of the feet is significantly thicker than the skin on the face or neck. Thicker skin often requires deeper sutures and longer healing times, which increases the window for potential complications. Conversely, very thin skin, such as that on the shins or the tops of the hands, lacks the underlying fatty cushion found elsewhere, making scars appear more recessed or tethered to the bone.
The presence of sebaceous glands and hair follicles also influences how a scar forms and how it responds to treatment. Areas with a high concentration of oil glands, like the nose or the center of the back, are more prone to inflammatory responses. If an incision becomes clogged with oils or bacteria during the early stages of healing, the resulting inflammation can degrade the quality of the scar. This is why skin prep and post-operative hygiene are so critical in these specific regions.
To better understand the steps involved in treating a complex scar in a difficult anatomical location, consider the following sequential process:
- Pre-treatment Priming: Using medical-grade topicals to optimize skin health and reduce inflammation before any revision is attempted.
- Surgical Revision: Carefully excising the old scar tissue and performing a multi-layered closure to offload surface tension.
- Incision Stabilization: Applying specialized tapes or glues that provide external support to the wound edges for the first several weeks.
- Laser Refinement: Utilizing vascular or resurfacing lasers once the scar is closed to reduce redness and smooth out the texture.
- Long-term Compression: Implementing silicone therapy or compression sleeves to keep the scar flat and hydrated during the remodeling phase.
This step-by-step approach ensures that every variable is controlled. In areas like the lower legs, where gravity and venous pressure can cause scars to turn purple or brown, additional steps like compression therapy are vital. The skin in these distal regions does not regenerate as quickly as the skin on the scalp or face, meaning the maturation process can take up to two years. Patience is a necessary component of the treatment plan for any scar located below the waist.
Dr. Kohan emphasizes that while some areas are more difficult, none are impossible to improve. The key is to match the treatment to the specific biological needs of the site. For example, a scar on the thin skin of the hand might benefit more from fat grafting to provide volume, while a thick scar on the back might require steroid injections to soften the collagen. At EmilMD, the team uses a diverse toolkit to address these varied challenges, ensuring that every patient receives a personalized solution.
By combining surgical precision with advanced dermatological treatments, the practice can achieve outcomes that were previously thought unattainable in high-tension areas. The integration of laser technology, such as IPL for redness or CO2 for texture, allows for a level of refinement that surgery alone cannot provide. This multi-modal strategy is especially effective for scars that have already failed traditional treatments elsewhere.
The Role of Pigmentation and Blood Supply in Healing
The visibility of a scar is often determined by its color, which is a reflection of the blood supply and melanocyte activity in that specific area. The face and neck have a very rich vascular network, which is why they heal so quickly. However, this same blood supply can cause scars in these areas to remain red or pink for a longer duration. In contrast, areas with less robust circulation, such as the ankles or the middle of the back, may heal more slowly and are at a higher risk for hyperpigmentation or dark staining.
Pigmentation issues are particularly challenging in patients with darker skin tones, as the inflammation of a scar can trigger an overproduction of melanin. This results in post-inflammatory hyperpigmentation, where the scar appears much darker than the surrounding skin. Treating these scars requires a delicate balance, as aggressive treatments can sometimes trigger even more pigment production. Specialists must use a "low and slow" approach, utilizing gentle peels and specific laser settings to gradually even out the skin tone. Here are some examples of how different areas respond based on their unique physiological characteristics:
- Face and Scalp: Fast healing due to excellent blood supply but prone to prolonged redness.
- Neck and Jawline: Good healing potential but susceptible to stretching if the underlying muscles are active.
- Abdomen: Generally heals well, though tension from weight fluctuations or core movement can widen the scar.
- Extremities: Slower healing and higher risk of pigmentation changes due to distance from the heart.
- Hands and Feet: Difficult to treat because of the thin skin and constant exposure to the environment.
Because the blood supply varies so much, the timing of suture removal also varies by body part. Sutures on the face may be removed in as little as five days to prevent "railroad track" marks, while sutures on the back or legs may need to stay in for two weeks or more. This nuance in clinical decision-making is vital for a successful outcome. At EmilMD, every post-operative schedule is customized to the specific anatomical site of the procedure.
The psychological burden of scarring is often tied to these visible locations. A scar on the face, even if technically "well-healed," can feel more difficult for a patient than a larger scar on the hip. Dr. Kohan understands the emotional impact of these marks and strives to provide results that allow patients to feel comfortable in their own skin. By addressing the redness and pigmentation early, the team can help the scar fade into the background more quickly.
For those dealing with scars in difficult areas, the most important thing is to seek expert advice early. Waiting too long can allow a scar to become "fixed" in its appearance, making it more resistant to non-surgical treatments. The clinical team at EmilMD is adept at intervening during the active remodeling phase to steer the scar toward a flatter, paler, and more discreet state. Through a combination of clinical excellence and patient education, the practice helps individuals navigate the complexities of wound healing.
Advanced Strategies for Managing Complex Scar Tissue
When standard treatments are not enough to address a difficult scar, advanced surgical and non-surgical strategies must be employed. One such method is the use of tissue expansion, which allows the surgeon to grow extra healthy skin near a scar to replace the damaged area. This is particularly useful for large scars on the scalp or limbs where there is not enough local skin to perform a simple revision. While it is a longer process, the results are often superior because the new skin perfectly matches the color and texture of the surrounding area.
Another powerful tool in the management of difficult scars is the use of fractional lasers and microneedling with radiofrequency. These technologies create thousands of microscopic zones of injury within the scar tissue, triggering a fresh healing response. By breaking up the dense, disorganized collagen of an old scar and replacing it with new, organized fibers, these treatments can significantly improve both flexibility and appearance. This is especially beneficial for scars over joints that have become tight and restrictive.
To summarize the various ways modern medicine tackles these tough cases, the following details advanced options:
- Z-Plasty Technique: A surgical maneuver that changes the direction of a scar to align it with natural skin folds and reduce tension.
- Fat Grafting: Injecting the patient's own fat beneath a tethered or depressed scar to provide cushioning and improve skin quality.
- Steroid Impregnated Tape: A specialized adhesive that delivers a consistent dose of medication to flatten raised, itchy scars on the chest or shoulders.
- Vascular Laser Therapy: Targetting the tiny blood vessels within a red scar to "starve" the excess collagen and allow the mark to fade.
These techniques are most effective when used as part of a comprehensive plan. At EmilMD, the focus is not just on the scar itself but on the overall health of the skin and the patient's lifestyle. For example, a patient who smokes will have a much harder time healing in any area of the body because nicotine constricts blood vessels and reduces oxygen delivery to the wound. Addressing these systemic factors is just as important as the physical treatment of the scar.
The evolution of scar management has moved away from a "one size fits all" mentality. We now understand that the biology of a scar is a dynamic process that lasts for years. This means that even an old scar can often be improved with the right combination of modern interventions. Whether it is through surgical re-alignment or the use of cutting-edge lasers, the goal is always to restore as much of the original form and function as possible.
Dr. Kohan and his clinical team at EmilMD remain at the forefront of these developments, constantly refining their protocols to offer the best possible care. They understand that every scar tells a story, but it does not have to be the most prominent part of a person's appearance. By utilizing the full spectrum of available treatments, the practice helps patients move past the physical and emotional reminders of past injuries or surgeries.
Optimizing Long-Term Outcomes through Professional Guidance
Achieving the best possible outcome for a scar in a difficult area requires a long-term commitment to care. The maturation process of a scar is not measured in weeks but in months and years. During this time, the tissue is constantly remodeling and changing its structure. Professional guidance is essential to ensure that this remodeling proceeds in a favorable direction. Regular follow-up appointments allow the surgeon to monitor the scar's progress and intervene if signs of hypertrophy or widening appear.
Patient education is a cornerstone of this long-term success. Understanding why certain activities must be limited or why a specific topical must be applied daily empowers the patient to take an active role in their healing. At EmilMD, the staff takes the time to explain the science behind each recommendation, ensuring that the patient feels supported throughout the entire process. This collaborative approach leads to higher patient satisfaction and superior aesthetic results.
Key takeaways for managing scars in difficult body areas include:
- Early Intervention: Addressing a scar during the active healing phase is more effective than waiting until it is fully matured.
- Tension Management: Using tapes, sheets, and activity modification to protect scars in high-motion areas like the shoulders and joints.
- Sun Protection: Keeping scars out of the sun for at least a year to prevent permanent darkening and pigment issues.
Providing practical clarity for patients helps manage expectations and reduces the anxiety often associated with scarring. While some areas of the body are inherently more difficult to treat, modern plastic surgery offers a wealth of options to mitigate these challenges. Dr. Kohan's expertise in anatomical nuances ensures that even the most stubborn scars can be improved with the right plan.
The most important factor in scar management is the skill and experience of the provider. Choosing a board-certified plastic surgeon who understands the intricacies of skin tension and wound healing makes a significant difference in the final result. At EmilMD, the dedication to clinical excellence and patient-centered care ensures that every scar, no matter where it is located, is treated with the highest level of precision and compassion. By focusing on both the science of healing and the art of aesthetics, the practice delivers results that truly enhance the patient's quality of life.
Frequently
Asked Questions
Why do scars on my chest look different than scars on my face?
The skin on your chest is under significantly more tension than the skin on your face, and it also has a different blood supply and thickness. Because the chest is constantly moving as you breathe and use your arms, the body often produces extra collagen to keep the wound from pulling apart, which can result in a raised or thickened appearance. The experts at EmilMD note that the face has a very high density of blood vessels, which allows for much faster and more discreet healing compared to the trunk of the body.
Can a keloid scar be permanently removed from the shoulder?
Removing a keloid from a high-tension area like the shoulder is a complex process because the original trauma of surgery can actually trigger a new keloid to form. However, Dr. Emil Kohan’s expert team uses a specialized combination of surgical excision and immediate follow-up treatments, such as steroid injections or pressure therapy, to significantly reduce the risk of recurrence. While keloids are inherently difficult to treat, the multi-modal approach used at EmilMD provides the best possible chance for a flat and stable result.
Does smoking really affect how a scar heals on my legs?
Smoking has a profound impact on wound healing throughout the body, but it is especially detrimental to scars on the lower extremities where circulation is already naturally slower. Nicotine causes blood vessels to constrict, which starves the healing tissue of the oxygen and nutrients it needs to repair itself properly. At EmilMD, patients are strongly advised to quit smoking before and after any procedure to prevent complications like skin necrosis or widened, poor-quality scars. Dr. Emil Kohan emphasizes that optimal blood flow is the single most important factor in achieving a thin, healthy scar.
Is it possible to improve a very old scar that has already turned white?
Yes, even old, white scars, known as mature or hypopigmented scars, can often be improved with modern clinical techniques. While the color can be difficult to change completely, the texture and thickness can be refined using fractional CO2 lasers or microneedling to stimulate new collagen growth. The team at EmilMD often uses these energy-based devices to blend the scar more effectively with the surrounding skin, making it much less noticeable. Dr. Kohan can evaluate the age and type of your scar to determine which resurfacing method will offer the most benefit.
How long should I wait after surgery before starting laser scar treatments?
The timing for laser treatment depends on the specific type of laser being used and the anatomical location of the scar. In many cases, vascular lasers can be used just a few weeks after surgery to reduce redness, while resurfacing lasers are typically used once the scar has gained more structural strength, usually around three to six months. At EmilMD, the clinical team monitors your healing progress closely to identify the ideal window for starting these supplemental treatments. Starting too early can disrupt the healing process, while waiting too long might miss the most active phase of remodeling.
Are there certain skin types that are more prone to difficult scarring?
Individual genetics and skin tone play a significant role in how the body responds to injury, with some people being naturally "heavy scarriers." Patients with darker skin tones are often more susceptible to keloids and post-inflammatory hyperpigmentation, which requires a more cautious and specialized treatment approach. Dr. Emil Kohan is highly experienced in treating a diverse range of skin types and tailors his surgical and post-operative protocols to minimize these risks. Whether you have very fair skin or a deep complexion, EmilMD provides the specialized care necessary to ensure your scars heal as beautifully as possible.